Showing 1 - 9 of 17 articles

Unmasking Big Tobacco: an open letter to all Australians
Australia has some of the lowest smoking rates in the world - the result of decades of evidence-based policies that have saved lives.

Tradies beware: Five workplace cancer risk factors
Although Australia’s trade industry makes up less than one-third of our workforce, it accounts for 58 per cent of serious claims for worker’s compensation and over two-thirds of work-related traumatic injury fatalities in Australia. Being a tradie clearly carries risks. However, something that is not entirely reflected in these statistics is the burden of work-related cancers. It is estimated that approximately 6.5 percent of new cancer cases diagnosed in Australia every year are caused by workplace risk factors. This amounts to around 5000 workplace cancers every year! Tradies are among those who are most likely to be exposed to carcinogens (cancer-causing agents) while at work. That’s why, this Tradies National Health Month we are urging Australian tradies to be aware of the carcinogens they can be exposed to at work, and to always use appropriate control measures to protect themselves. Here are five common cancer risk factors tradies need to be aware of in the workplace:

How to prepare for a telehealth consultation
As our healthcare system adapts to COVID-19, a key change has been the transition of many appointments to telehealth. Telehealth appointments are currently operating in several different ways. Sometimes it is a telephone call from your doctor to you at home, sometimes it is a video conference from your home to your doctor. Other times, you might go in to see your regular GP in person, and then connect with a specialist remotely via video.

12 tips to reduce your alcohol intake
Drinking alcohol is a big part of Australia’s social culture – but unfortunately, it’s to the detriment of our nation’s health. Many Australians aren’t aware of the link between alcohol consumption and cancer, despite convincing evidence that drinking alcohol increases the risk of 7 types of cancer – including cancers of the mouth, liver, bowel and breast.

The birth of Slip, Slop, Slap and the science behind nation-wide behaviour change
Former Cancer Council Victoria CEO, David Hill, shares how science was used to change a nation's attitude towards skin cancer and its prevention with iconic programs and campaigns such as ‘Slip, Slop, Slap,’ and ‘Timebomb.’
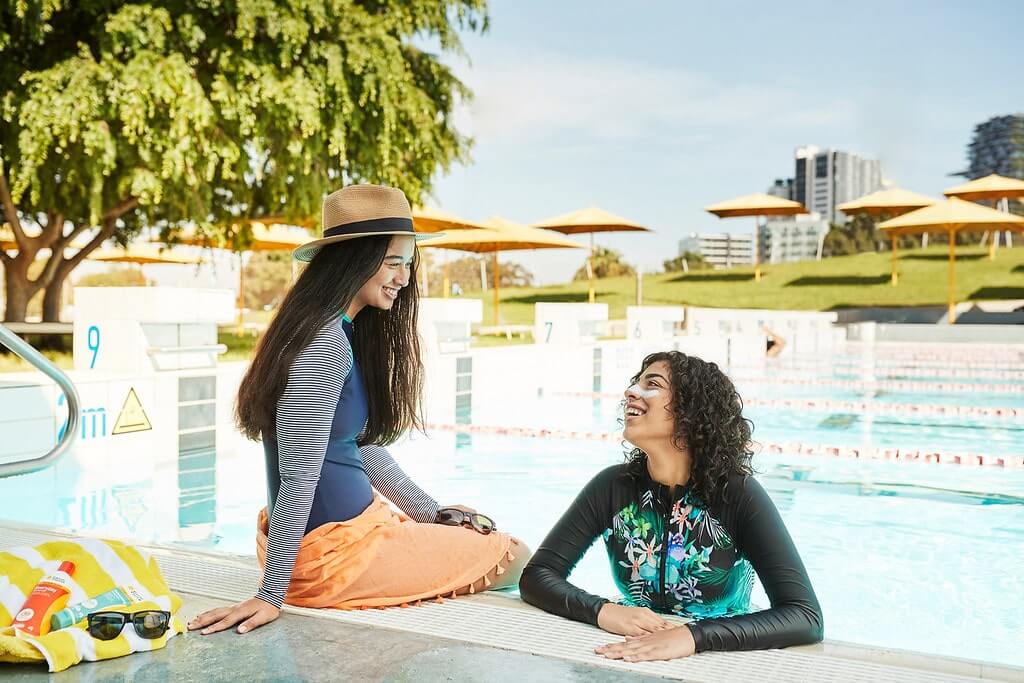
What happens to your skin when you get sunburnt? A dermatologist explains
Too many Australians pay with their lives for their past sun exposure, with over 2000 dying from skin cancer each year. The good news is skin cancer is primarily a preventable cancer. That’s why this week, as part of National Skin Cancer Action Week, we are urging Australians to be aware that the sunburn you suffer when you are young can lead to skin cancer further down the track.

5 workplace cancer risks you may not be aware of
You may be aware that some lifestyle factors such as smoking or alcohol can cause cancer, but are you aware of potential cancer risks in your workplace? In Australia, sadly around 5000 work-related cancers are diagnosed each year.

Cancer, your work and you: should you tell your employer and colleagues about your diagnosis?
When you are first diagnosed with cancer there are usually a million things running through your mind. As well as trying to come to terms with the news, getting information about your diagnosis and treatment, and thinking about how to tell loved ones, the question often arises - what about work?

Every cancer patient should be prescribed exercise medicine
Every four minutes someone in Australia is diagnosed with cancer. Only one in ten of those diagnosed will exercise enough during and after their treatment. But every one of those patients would benefit from exercise.
Showing 1 - 9 of 17 articles
