Last updated:
Sources and references For many people, lung cancer is diagnosed at an advanced stage. In these cases, the main goal of treatment is to manage symptoms for as long as possible. This chapter describes procedures and strategies for managing the most common symptoms of lung cancer. Keep in mind that you won’t necessarily experience every symptom listed here.
Breathlessness
Many people with lung cancer have difficulty breathing before or after diagnosis. This shortness of breath is also called breathlessness or dyspnoea. It can occur for several reasons, including:
- the cancer itself and lungs not working as well
- drop in fitness level due to less physical activity
- build-up of fluid (pleural effusion) in the pleural cavity, the space between the 2 layers of thin tissue covering the lung
- lung tissue changes after radiation therapy (radiation pneumonitis)
- other respiratory conditions, such as COPD.
If the cancer is blocking a main airway, a laser, stent (a metal or plastic tube) or radiation therapy may help open the airway and make breathing easier. You may also be referred to a pulmonary rehabilitation program to learn how to manage breathlessness. This program will include exercise, breathing techniques, ways to clear the airways, and tips for conserving energy. Some people also use supplemental oxygen at home.
If you smoke or vape, your doctor will recommend you quit and suggest ideas for how to do this.
Having a pleural tap
For some people, fluid may build up in the pleural cavity, the space between the 2 layers of thin tissue covering the lung. The build-up of fluid is called pleural effusion. This can put pressure on the lung, making it hard to breathe. Having a pleural tap can relieve this symptom. This procedure is also known as pleurocentesis or thoracentesis.
To drain the fluid, your doctor or radiologist numbs the area with a local anaesthetic and inserts a hollow needle between your ribs into the pleural cavity. It then takes about 30–60 minutes to drain the fluid. You usually don’t have to stay overnight in hospital after a pleural tap. A sample of the fluid is sent to a laboratory for testing.
Having a pleural tap
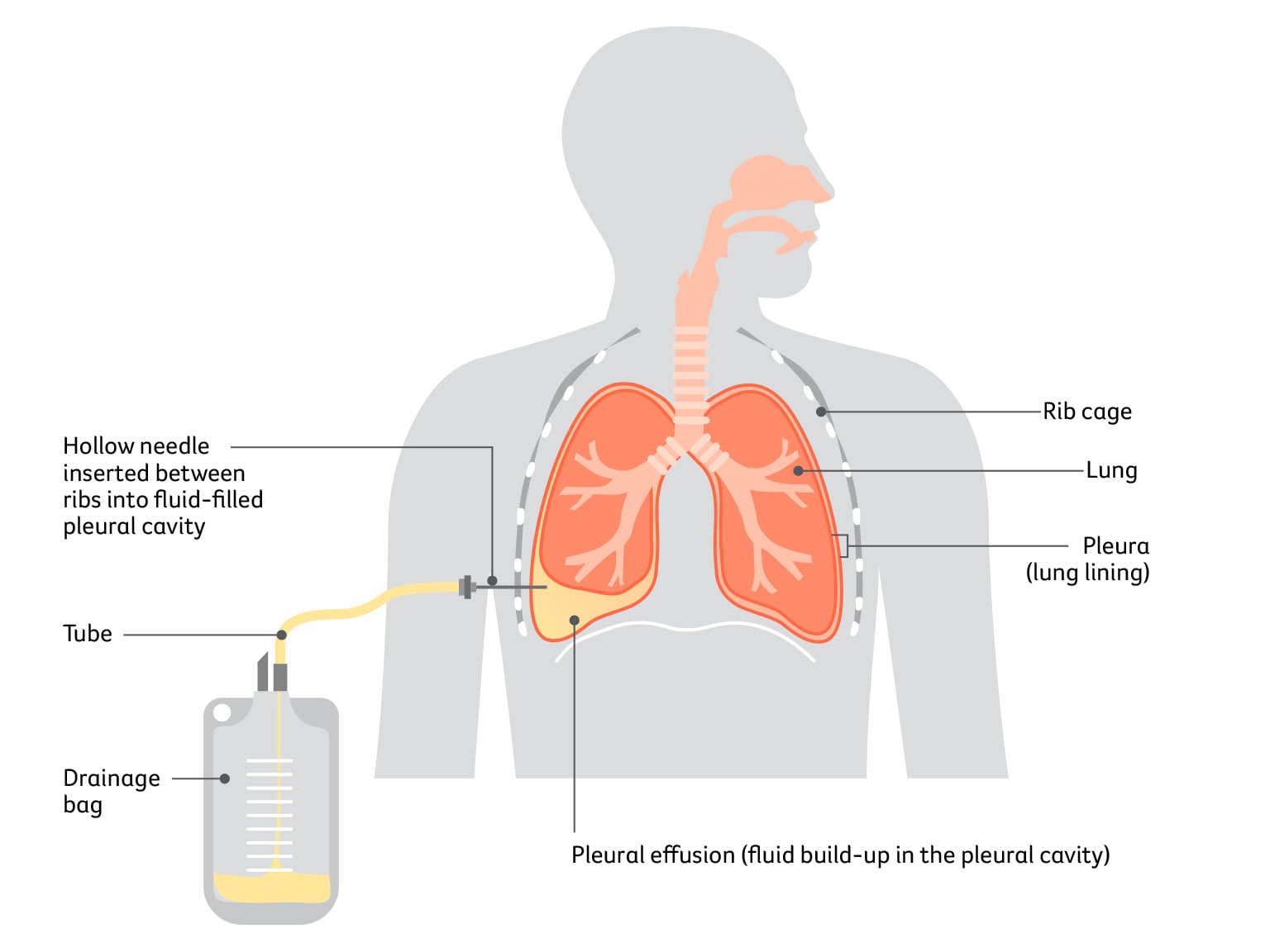
Ways to control fluid around the lungs
If breathlessness is caused by pleural effusion, you may need to have surgery.
Types of procedures include:
- pleural tap to drain the fluid
- pleurodesis to stop fluid building up again
- an indwelling pleural catheter.
Pleurodesis
Pleurodesis is a way to close the pleural cavity. Your doctors might recommend this procedure if the fluid builds up again after you have had a pleural tap. It may be done by a thoracic surgeon or respiratory physician in one of two ways, depending on how well you are and what you would prefer.
VATS pleurodesis – This method uses a keyhole approach called video-assisted thoracoscopic surgery (VATS). You will be given a general anaesthetic, then the surgeon will make one or more small cuts in the chest and pass a tiny video camera and operating instruments through.
After all fluid has been drained, the surgeon then injects some sterile talcum powder into the pleural cavity. This causes inflammation that helps stick the 2 layers of the pleura together and prevents fluid from building up again. You will stay in hospital for a few days.
Bedside talc slurry pleurodesis – If you are unable to have a general anaesthetic, apleurodesis can be done under local anaesthetic. A small cut is made in the chest, then a tube is inserted into the pleural cavity. Fluid can be drained through the tube into a bottle.
Next, sterile talcum powder mixed with salt water (a “slurry”) is injected through the tube into the pleural cavity. Nurses will help you move into various positions every 10 minutes to get the talc slurry to spread throughout the pleural cavity. The process takes about an hour.
A talc slurry pleurodesis usually requires a stay in hospital of 2–3 days. After the procedure, some people feel a burning pain in the chest for 1–2 days, but this can be eased with medicines.
Indwelling pleural catheter
An indwelling pleural catheter is a small soft tube used to drain fluid from around the lungs. It may be offered if fluid keeps building up in the pleural cavity making it hard to breathe, or if you are unable or do not want to have a pleurodesis. The catheter can be in place permanently, or until it is no longer needed.
You will be given a local anaesthetic, then the doctor makes 2 small cuts in the chest wall and inserts the catheter into the pleural cavity. One end of the tube is inside the chest, and the other is coiled and fixed outside your skin with a small dressing.
The fluid can be drained at home. When fluid builds up and needs to be drained (usually once or twice a week), the catheter is connected to a small bottle. A community nurse can drain the fluid for you or they can teach you, a family member or friend how to drain the catheter.

Pain
Pain can be a symptom of lung cancer and a side effect of treatment. If pain is not controlled, it can affect your quality of life and how you cope with treatments.
There are different ways to control pain. Aside from pain medicines, various procedures can manage any build-up of fluid that is causing pain. Radiation therapy and chemotherapy can reduce pain by shrinking a lung tumour. Surgery may help treat pain from bones: for example, if the cancer has spread to the spine and is pressing on nerves (nerve compression).
Poor appetite and weight loss
Some people stop feeling interested in eating and lose weight before lung cancer is diagnosed. These symptoms may be caused by the disease itself, or by feeling sick, having difficulty swallowing, being breathless, or feeling down.
Weight loss can affect how your body responds to cancer treatment, your risk of infection, and how quickly you recover. This can happen to anyone, no matter what size. Eating well will help you cope better with treatment and side effects, and improve your quality of life.
Fatigue
It is common to feel very tired during or after treatment, and you may not have the energy for day-to-day activities. Cancer-related fatigue is different from tiredness, as it may not go away with rest or sleep. You may also lose interest in things that you usually enjoy doing or have trouble concentrating on one thing for very long.
Let your treatment team know if you are struggling with fatigue. Sometimes fatigue can be caused by a low red blood cell count (anaemia), or be a side effect of drug therapies or a sign of depression, all of which can be treated. There are also many hospital and other programs available to help you manage fatigue.
Difficulty sleeping
Getting a good night’s sleep is important for maintaining your energy levels, reducing fatigue and improving your mood. Pain, breathlessness, anxiety, depression and some medicines can make it hard to sleep. If you already had sleep problems before the lung cancer diagnosis, these could become worse.
Talk to your doctor about what might help improve your ability to sleep. Your medicines may need adjusting, or sleep medicines may be an option. Talking to a counsellor may help if you are feeling anxious or depressed. Some strategies that people with cancer have found helpful are listed below.
Key points about managing lung cancer symptoms
Shortness of breath
Breathlessness can be managed with:
- surgical procedures – including pleural tap to drain fluid, pleurodesis to stop fluid building up again, and an indwelling pleural catheter to drain fluid
- pulmonary rehabilitation – including exercise training and breathing techniques
- medicines – such as low doses of morphine
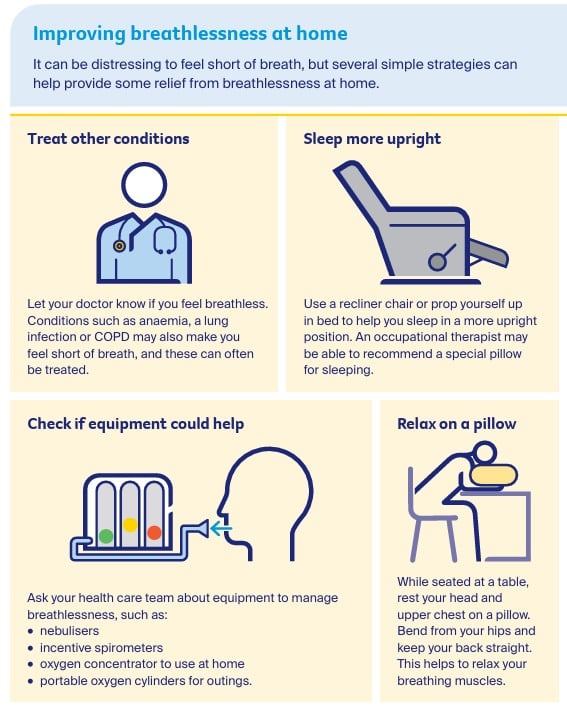
- self-management strategies – such as using a handheld fan, sleeping upright, gentle exercise, positioning pillows and relaxation techniques.
Pain
Pain can be managed with:
- pain medicines
- procedures that drain fluid or reduce the size of the cancer
- radiation therapy or chemotherapy
- self-management strategies – such as keeping a symptom diary, and learning relaxation and meditation techniques.
Other symptoms
Many people with lung cancer also experience:
- poor appetite and weight loss – see a dietitian for ways to make food nutritious and appealing
- fatigue – pace yourself, accept help and find ways to exercise; an exercise physiologist or physiotherapist can prepare a suitable exercise plan for you and an occupational therapist can help you learn ways to manage fatigue and conserve energy
- difficulty sleeping – try to do some gentle physical activity every day, avoid watching television or looking at a computer, smartphone or tablet before bed, and have a set bedtime routine.
Looking after yourself
Cancer can cause physical and emotional strain, so it’s important to look after your wellbeing. Cancer Council has free booklets and programs to help you during and after treatment. Call 13 11 20 to find out more, or visit your local Cancer Council website.
Eating well
Healthy food can help you cope with treatment and side effects. A dietitian can explain how to manage any special dietary needs or eating problems and choose the best foods for your situation.
Staying active
Physical activity can reduce tiredness, improve circulation and lift mood. The right exercise for you depends on what you are used to, how you feel, and your doctor’s advice.
Complementary therapies
Complementary therapies are designed to be used alongside conventional medical treatments. Therapies such as massage, relaxation and acupuncture can increase your sense of control, decrease stress and anxiety, and improve your mood. Let your doctor know about any therapies you are using or thinking about trying, as some may not be safe or evidence-based.
Work and money
Cancer can change your financial situation, especially if you have extra medical expenses or need to stop working. Getting professional financial advice and talking to your employer can give you peace of mind. You can also check whether any financial assistance is available to you by asking a social worker at your hospital or treatment centre or calling Cancer Council 13 11 20.
Relationships
Having cancer can affect your relationships with family, friends and colleagues in different ways. Cancer is stressful, tiring and upsetting, and this may strain relationships. The experience of cancer may also result in positive changes to your values, priorities or outlook on life. Give yourself time to adjust to what’s happening, and do the same for those around you. It may help to discuss your feelings with each other.
Sexuality
Cancer can affect your sexuality in physical and emotional ways. The impact of these changes depends on many factors, such as treatment and side effects, your self-confidence, and if you have a partner. Although sexual intercourse may not always be possible, closeness and sharing can still be part of your relationship.
Contraception and fertility
If you can have sex, you may need to use certain types of contraception to protect your partner or avoid pregnancy for a time. Your doctor will explain what precautions to take. They will also tell you if treatment will affect your fertility permanently or temporarily. If having children is important to you, discuss the options with your doctor before starting treatment.
Sources and references
This edition has been developed by Cancer Council NSW on behalf of all other state and territory Cancer Councils as part of a National Cancer Information Subcommittee initiative. We thank the reviewers of this booklet: Dr Malinda Itchins, Thoracic Medical Oncologist, Royal North Shore Hospital and Chris O’Brien Lifehouse, NSW; Dr Cynleen Kai, Radiation Oncologist, GenesisCare, VIC; Dr Naveed Alam, Thoracic Surgeon, St Vincent’s Hospital, Epworth Richmond, and Monash Medical Centre, VIC; Helen Benny, Consumer; Dr Rachael Dodd, Senior Research Fellow, The Daffodil Centre, NSW; Kim Greco, Specialist Lung Cancer Nurse Consultant, Flinders Medical Centre, SA; Caitriona Nienaber, 13 11 20 Consultant, Cancer Council WA; Marco Salvador, Consumer; Janene Shelton, Lung Foundation Australia – Specialist Lung Cancer Nurse, Darling Downs Health, QLD; Prof Emily Stone, Respiratory Physician, Department of Thoracic Medicine and Lung Transplantation, St Vincent’s Hospital Sydney, NSW; A/Prof Marianne Weber, Stream Lead, Lung Cancer Policy and Evaluation, The Daffodil Centre, NSW. We would also like to thank the health professionals, consumers and editorial teams who have worked on previous editions of this title.
Cancer Council 13 11 20
Call us to talk to a specially trained health professional for free and confidential support and information.
Guide to best cancer care
This lung cancer guide explains the standard of high-quality cancer care that all Australians can expect, from diagnosis, to treatment, recovery, and living with cancer.



