Last updated:
Sources and references This page details the 2 most common types of skin cancer – basal cell carcinoma (BCC) and squamous cell carcinoma (SCC). These skin cancers are called non-melanoma skin cancer or keratinocyte cancer. For information about melanoma, see our page about melanoma.
What causes skin cancer?
More than 95% of skin cancers are caused by exposure to UV radiation. When unprotected skin is exposed to UV radiation, how the cells look and behave can change.
Australia has one of the highest UV levels in the world. The UV peaks during summer, but can damage unprotected skin most of the year. Even moderate UV levels can still do damage. UV radiation can’t be seen or felt. It isn’t related to the temperature and can still be high on cloudy days. UV radiation can cause sunburn; premature skin ageing; and damage to skin cells, which can lead to skin cancer.
You can’t always see sun damage that’s happened to the skin – and it can happen long before you get sunburnt or develop a tan. The damage also adds up over time and can’t be reversed.
You can check the UV levels in your local area on the SunSmart Global UV app. For information on how to properly protect your skin from the sun and prevent skin cancer
How common is skin cancer?
Australia has one of the highest rates of skin cancer in the world. About 2 out of 3 Australians will be diagnosed with some form of skin cancer before the age of 70.
Non-melanoma (keratinocyte) skin cancer is the most common cancer diagnosed in Australia. Over 1 million treatments are given each year in Australia for non-melanoma skin cancers. BCC can develop in young people, but it is more common in people over 40. SCC occurs mostly in people over 50.
Who is at risk?
Anyone of any age can develop skin cancer but it becomes more common as you get older. Many factors can increase your risk of skin cancer, including having:
- pale or freckled skin, especially if it burns easily and doesn’t tan
- red or fair hair and light-coloured eyes (blue or green)
- unprotected exposure to UV radiation, particularly a pattern of short, intense periods of sun exposure and sunburn, such as on weekends and holidays
- actively tanned, sunbaked or used solariums
- worked outdoors or spent a lot of time outside (e.g. gardening or golfing)
- been exposed to arsenic
- a weakened immune system – this may be from having leukaemia or lymphoma or using medicines that suppress the immune system (e.g. for rheumatoid arthritis, another autoimmune disease or for an organ transplant)
- lots of moles, or lots of moles with an irregular shape and uneven colour
- a previous skin cancer or family members with a history of skin cancer
- certain skin conditions such as sunspots because it shows that you have had a lot of skin damage from exposure to the sun.
People with brown, black, olive or very dark skin often have more protection against UV radiation, because their skin produces more melanin than fair skin does. However, people with darker skin can still develop skin cancer, sometimes in less sun-exposed areas of the body.
How to check your skin
In a room with good light, undress completely and use a full-length mirror to check your whole body. To check areas that are difficult to see, use a handheld mirror or ask someone to help you.
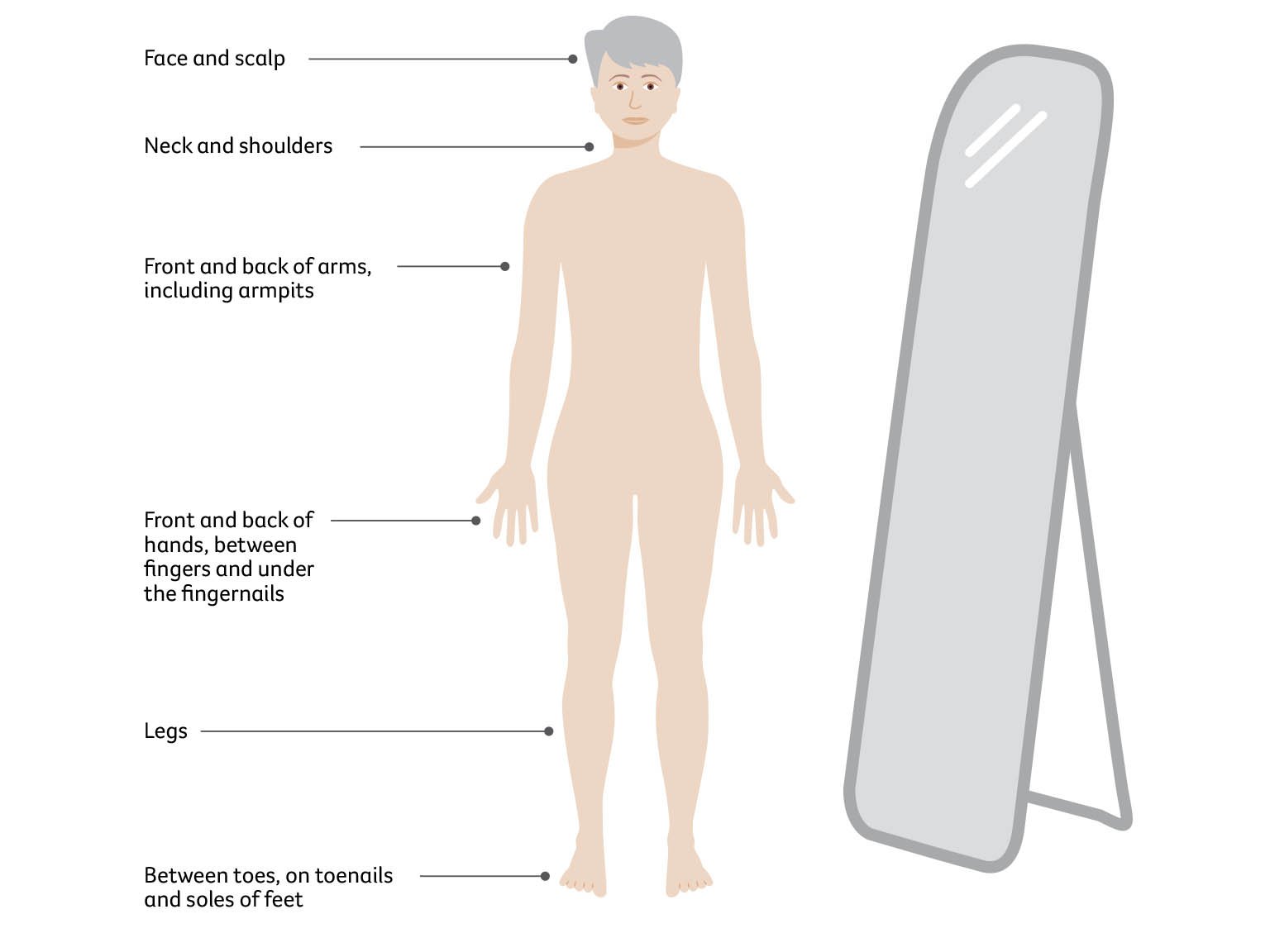
If there are any changes to your skin, if you notice something new, or you are worried about a spot you see, make an appointment with your doctor straightaway. You will have a better outcome if the skin cancer is found and treated early.
How do I spot a skin cancer?
Most skin cancers are self-detected. If you know what changes to watch for, you’ll be more likely to find a skin cancer early.
Skin cancers don’t all look the same, but there are some signs to look out for, including:
- a spot that looks and feels different from other spots on your skin
- a spot that has changed size, shape, colour or texture
- a spot that is tender or sore to touch
- a sore that doesn’t heal within a few weeks
- a sore that is itchy or bleeds.
Getting to know your skin will help you notice any new or changing spots. Make a time to regularly check your skin. You could try having a calendar reminder for the first day of the month, or you may want to do a check at the change of each season.
There is no set guideline on how often to check for skin cancer, but if you have had a skin cancer or are at greater risk of developing skin cancer, your doctor will do regular check-ups and will tell you how often you need to check your own skin.
Can smartphone apps help to detect skin cancer?
Some smartphone apps let you photograph your skin at regular intervals and compare the photos to check for changes. These apps may be a way to record any spot you are worried about or remind you to check your skin. However, research shows that apps cannot reliably detect skin cancer. If you notice a spot that worries you, make an appointment with your doctor straightaway.
Sources and references
This edition has been developed by Cancer Council NSW on behalf of all other state and territory Cancer Councils as part of a National Cancer Information Subcommittee initiative.
All updated content has been clinically reviewed by Prof Victoria Mar, Director, Victorian Melanoma Service, Alfred Hospital and Monash University, VIC and Prof Anne Cust, Acting Director, The Daffodil Centre, The University of Sydney and Cancer Council NSW, and faculty member, Melanoma Institute Australia.
This edition is based on the previous edition, which was reviewed by the following panel: Prof Victoria Mar (see above); Tracey Bilson, Consumer; Raelene Buchan, Consumer; Alison Button-Sloan, Consumer; Dr Margaret Chua, Radiation Oncologist, and the Skin Radiation Oncology team, Peter MacCallum Cancer Centre, VIC; Prof Anne Cust, (see above); A/Prof Paul Fishburn, Skin Cancer Doctor, Norwest Skin Cancer Centre, NSW and Faculty of Medicine, University of Queensland; Danielle Goss, Melanoma Clinical Nurse Specialist, Amie St Clair Melanoma (part of Melanoma Institute Australia), Wagga Wagga, NSW; Louise Pellerade, 13 11 20 Consultant, Cancer Council WA; Dr Shireen Sidhu, Head of Dermatology, The Royal Adelaide Hospital, SA; Dr Amelia Smit, Research Fellow – Melanoma and Skin Cancer, The Daffodil Centre, The University of Sydney and Cancer Council NSW; Dr Tony Tonks, Plastic and Reconstructive Surgeon, Canberra Plastic Surgery, ACT.
We also thank the health professionals, consumers and editorial teams who have worked on previous editions of this title.
Thanks also to Sydney Melanoma Diagnostic Centre for providing the dysplastic naevus photograph on page 11, A/Prof Paul Fishburn for providing the sunspot photograph on page 10, A/Prof Andrew Miller for providing the age spot photograph on page 10, and Prof H Peter Soyer for providing the other photographs on pages 9–11.
Cancer Council 13 11 20
Call us to talk to a specially trained health professional for free and confidential support and information.
Guide to best cancer care
This skin cancer guide explains the standard of high-quality cancer care that all Australians can expect, from diagnosis, to treatment, recovery, and living with cancer.



