Last updated:
Sources and references What's on this page
People with early NSCLC (stage 1 or 2) will generally be offered surgery to remove the tumour. How much of the lung is removed depends on several factors:
- the location and size of the cancer
- your general wellbeing and fitness
- how your lungs are working (lung function).
Surgery is not suitable for most people with advanced lung cancer.
If there is fluid in the pleural cavity (called pleural effusion) that keeps returning, you may have surgery (pleurodesis) to control this, or need to insert a catheter.
Preparing for treatment
Stop smoking
If you smoke or vape, you will be advised to stop before you start treatment for lung cancer.
Stopping smoking can improve how treatments work and reduce the impact of side effects such as breathlessness. Research shows that stopping smoking before surgery also reduces the chance of complications and can help you recover faster.
To work out a plan for stopping, talk to your doctor, your nurse specialist, or call Quitline on 13 7848 (13 QUIT).
Eat well and exercise
Your health care team may also suggest that you eat healthy foods and exercise before starting lung cancer treatment.
Preparing for treatment in this way is called prehabilitation. It can help you to cope with cancer treatment, recover more quickly and improve your quality of life.
A dietitian, exercise physiologist or physiotherapist can support you to make lifestyle changes. Ask your doctor for a referral.
Types of lung surgery
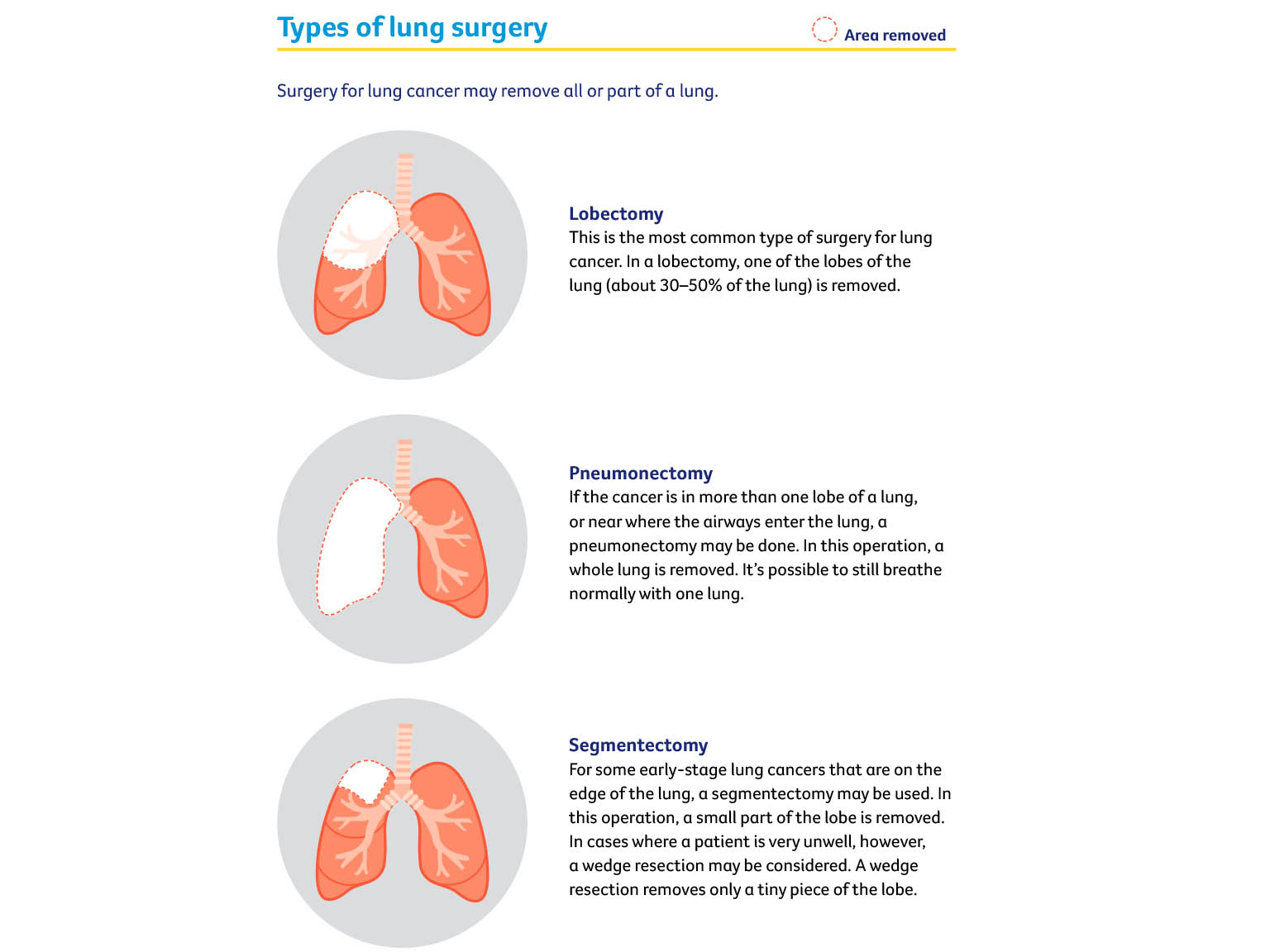
Removing lymph nodes
During surgery, the lymph nodes near the cancer will also be removed to check whether the cancer has spread. Knowing if the cancer has spread to the lymph nodes helps the doctors decide whether you need further treatment with chemotherapy or radiation therapy.
How the surgery is done
There are 2 main ways to perform surgery for lung cancer, and both require a general anaesthetic. Each type of surgery has advantages in particular situations – talk to your surgeon about the best option for you.
VATS – Lung cancer surgery can often be done using a keyhole approach. This is known as video-assisted thoracoscopic surgery (VATS). The surgeon will make a few small cuts (incisions) in the chest wall. A tiny video camera and operating instruments are passed through the cuts, and the surgeon performs the operation from outside the chest. A keyhole approach usually means a shorter hospital stay, faster recovery and fewer side effects.
Thoracotomy – If a long cut is made between the ribs in the side of the chest, the operation is called a thoracotomy. This may also be called open surgery. You will need to stay in hospital for 3–7 days. Sometimes the surgeon may need to change from a VATs approach to a thoracotomy during the surgery.
What to expect after surgery
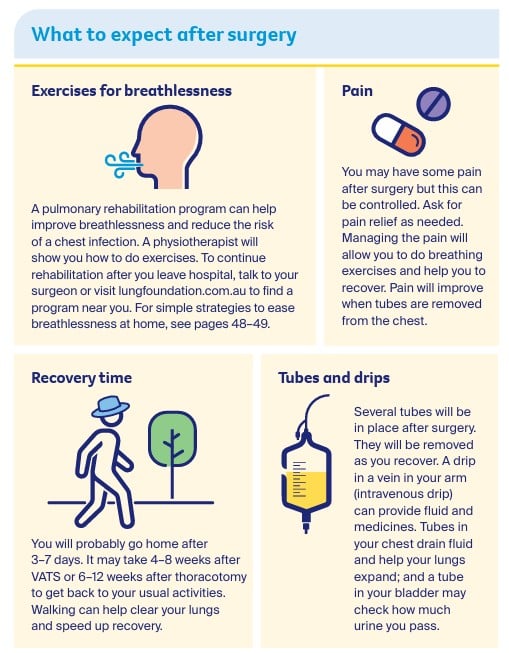
Find out more about the types of treatments:
Sources and references
This edition has been developed by Cancer Council NSW on behalf of all other state and territory Cancer Councils as part of a National Cancer Information Subcommittee initiative. We thank the reviewers of this booklet: Dr Malinda Itchins, Thoracic Medical Oncologist, Royal North Shore Hospital and Chris O’Brien Lifehouse, NSW; Dr Cynleen Kai, Radiation Oncologist, GenesisCare, VIC; Dr Naveed Alam, Thoracic Surgeon, St Vincent’s Hospital, Epworth Richmond, and Monash Medical Centre, VIC; Helen Benny, Consumer; Dr Rachael Dodd, Senior Research Fellow, The Daffodil Centre, NSW; Kim Greco, Specialist Lung Cancer Nurse Consultant, Flinders Medical Centre, SA; Caitriona Nienaber, 13 11 20 Consultant, Cancer Council WA; Marco Salvador, Consumer; Janene Shelton, Lung Foundation Australia – Specialist Lung Cancer Nurse, Darling Downs Health, QLD; Prof Emily Stone, Respiratory Physician, Department of Thoracic Medicine and Lung Transplantation, St Vincent’s Hospital Sydney, NSW; A/Prof Marianne Weber, Stream Lead, Lung Cancer Policy and Evaluation, The Daffodil Centre, NSW. We would also like to thank the health professionals, consumers and editorial teams who have worked on previous editions of this title.
Cancer Council 13 11 20
Call us to talk to a specially trained health professional for free and confidential support and information.
Guide to best cancer care
This lung cancer guide explains the standard of high-quality cancer care that all Australians can expect, from diagnosis, to treatment, recovery, and living with cancer.



