Last updated:
Sources and references Cancer of the uterus is usually treated with an operation that removes the uterus and cervix (total hysterectomy), along with both fallopian tubes and ovaries (bilateral salpingo-oophorectomy, see next page). If your ovaries appear normal, you don’t have any risk factors, and it is an early-stage, low-grade cancer, you may be able to keep your ovaries. If the cancer has spread beyond the cervix, the surgeon may also remove a small part of the upper vagina and the ligaments supporting the cervix.
Cancer of the uterus is usually treated with an operation that removes the uterus and cervix (total hysterectomy), along with both fallopian tubes and ovaries (bilateral salpingo-oophorectomy, see next page). If your ovaries appear normal, you don’t have any risk factors, and it is an early-stage, low-grade cancer, you may be able to keep your ovaries. If the cancer has spread beyond the cervix, the surgeon may also remove a small part of the upper vagina and the ligaments supporting the cervix.
Total hysterectomy and bilateral salpingo-oophorectomy
Most people with cancer of the uterus will have this operation, which removes the uterus, cervix, fallopian tubes and ovaries (as shown by the dotted line). Sometimes one or more pelvic lymph nodes are also removed to help with staging.
A pathologist examines all removed tissue and fluids. The results will help confirm the type of cancer of the uterus, if it has spread (metastasised), and its stage and grade. The cancer may also be tested for particular gene changes.
The surgery will be performed under a general anaesthetic. Your surgeon will discuss the most appropriate surgery for you, and explain the risks and benefits.
The type of hysterectomy you have depends on a number of factors, such as: your age and build; the size of your uterus; the tumour size; and the surgeon’s specialty and experience.
Keyhole surgery
Also called a laparoscopic hysterectomy, a surgeon inserts a laparoscope (thin tube with light and camera) and instruments through about 4 small cuts in the abdomen. The uterus and other organs are removed through the vagina.
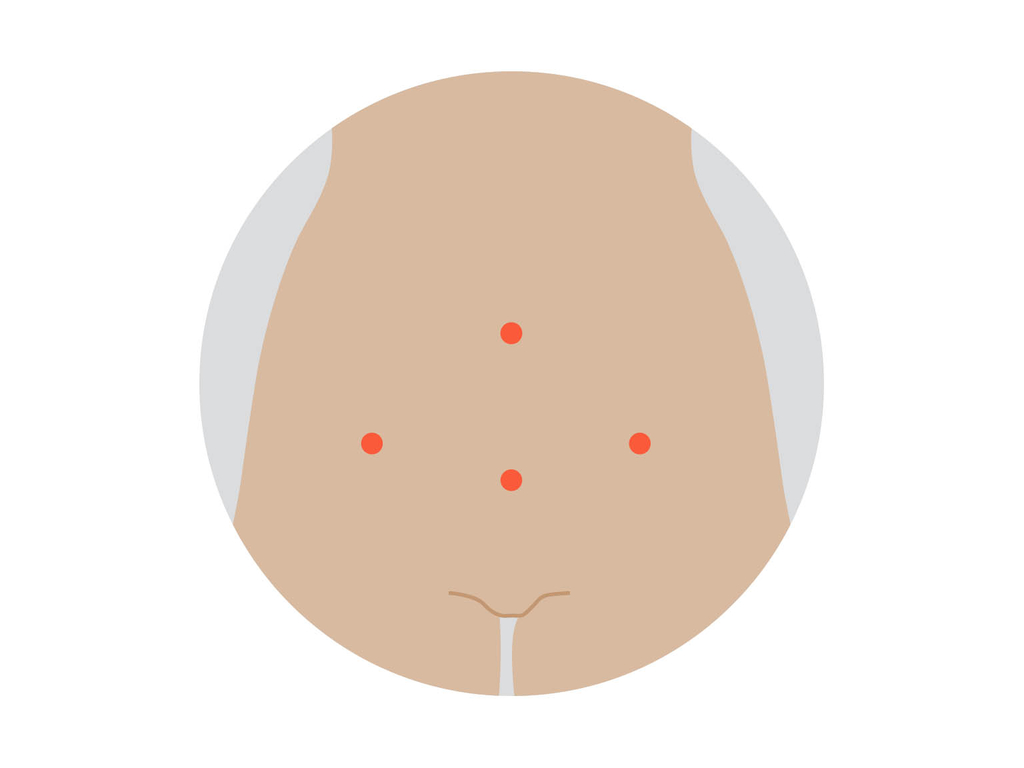
Robotic-assisted hysterectomy
This is a special form of keyhole surgery. The instruments and camera are inserted through about 4 small cuts, and controlled by robotic arms guided by the surgeon, who sits next to the operating table.
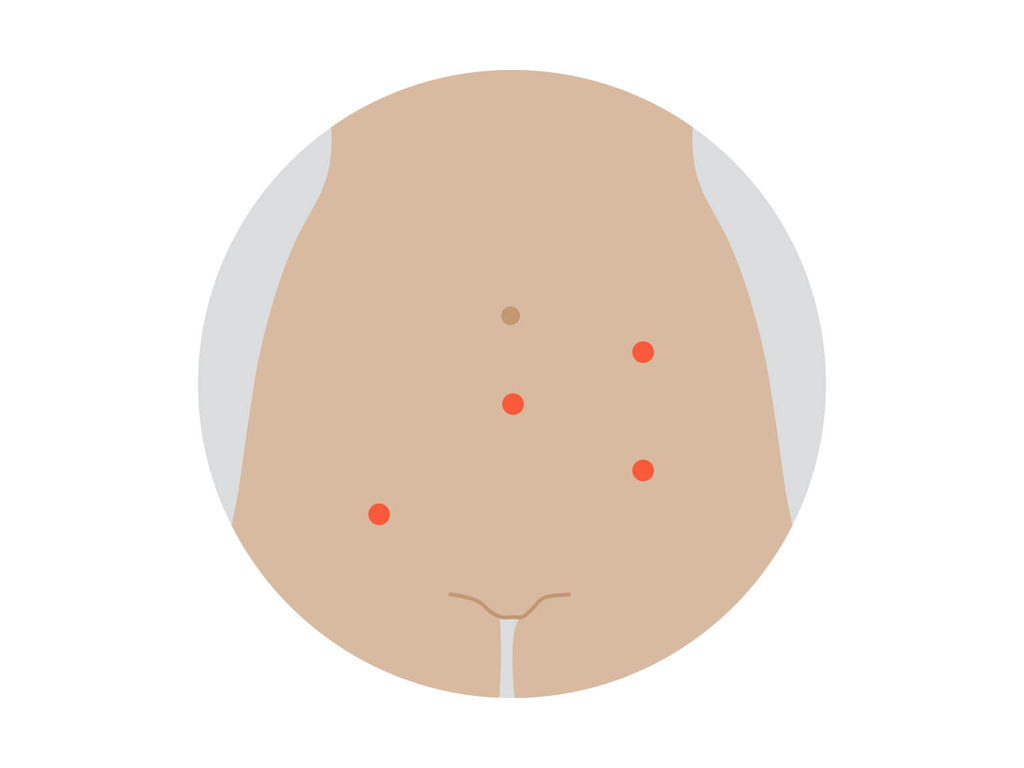
Open surgery
This surgery (also called abdominal hysterectomy or laparotomy) is done through the abdomen. A cut is usually made from the pubic area to the bellybutton. The uterus and other organs are then removed.
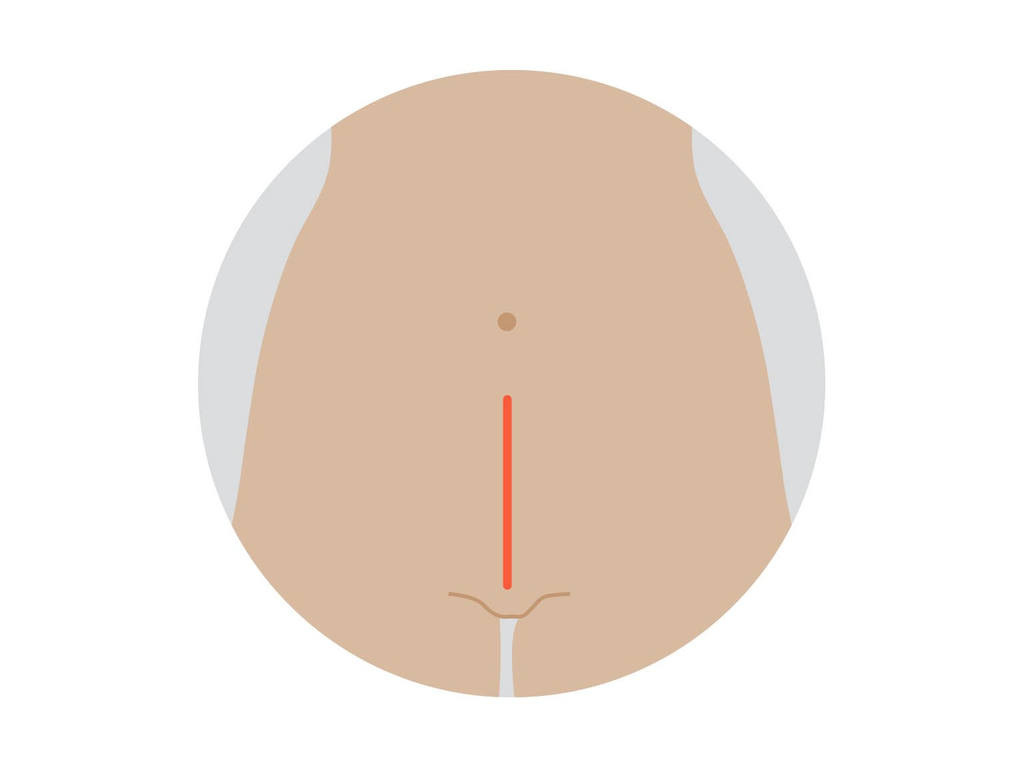
Treatment of lymph nodes
Cancer cells can spread from the uterus to the pelvic lymph nodes. If this occurs, your doctor may recommend you have additional treatment after surgery, such as chemotherapy or radiation therapy. Lymph nodes may be checked in 2 ways:
- Lymphadenectomy (lymph node dissection) – For more advanced or higher grade tumours, the surgeon may remove some lymph nodes from the pelvic area to see if the cancer has spread beyond the uterus.
- Sentinel lymph node biopsy – This test helps to identify the pelvic lymph node that the cancer is most likely to spread to first (the sentinel node). While you are under anaesthetic, your doctor will inject a dye into the cervix. The dye will flow to the sentinel lymph node, which will be removed for testing. Sentinel lymph node biopsies are available in most treatment centres.
What to expect after surgery
When you wake up after the operation, you will be in a recovery room near the operating theatre. Once you are fully conscious, you will be transferred to the ward.
Tubes and drips – You will have an intravenous drip in your arm to give you medicines and fluid, and a tube (catheter) in your bladder to collect urine (wee). These will usually be removed the day after the operation.
Length of stay – You will stay in hospital for about 1–4 days. How long you stay will depend on the type of surgery you had and how quickly you recover. Most people who have keyhole surgery will be able to go home on the first or second day after the surgery (and occasionally on the day of surgery).
Pain – As with all major surgery, you will have some discomfort or pain. The level of pain will depend on the type of operation. After keyhole surgery, you will usually be given pain medicine to swallow. If you have open surgery, you may be given pain medicine in different ways:
- through a drip into a vein (intravenously)
- via a local anaesthetic injection into the abdomen (a transverse abdominis plane or TAP block)
- via a local anaesthetic injection into your back, either into spinal fluid (a spinal) or into the space around spinal nerves (an epidural)
- with a patient-controlled analgesia (PCA) system, a machine that allows you to press a button for a measured dose of pain relief.
While you are in hospital, let your doctor or nurse know if you are in pain so they can adjust your medicines to make you as comfortable as possible. Do not wait until the pain is severe. After you go home, you can continue taking pain medicine as needed.
Wound care – You can expect some light vaginal bleeding after the surgery, which should stop within 2 weeks. Your treatment team will talk to you about how you can keep the wound/s clean to prevent infection once you go home.
Blood clot prevention – You will be given a daily injection of a blood thinner to reduce the risk of blood clots. Depending on your risk of clotting, you may be taught to give this injection to yourself so you can continue it for a few weeks at home. You may also be advised to wear compression stockings for up to 4 weeks to help the blood in your legs circulate well and prevent clots.
Constipation – The medicines used during and after surgery can cause constipation (difficulty having bowel movements). Talk to your treatment team about how to manage this – they may suggest medicines to help prevent or relieve constipation. Once your surgeon says you can
get out of bed, walking around can also help.
Test results – Your doctor will have all the test results about 2 weeks after the operation. Whether more treatment is necessary will depend on the type, stage and grade of the disease, and the amount of remaining cancer, if any. If the cancer is at a very early stage, you may not need further treatment."
I had a total hysterectomy and some of my lymph nodes were removed as well. Fortunately, the cancer hadn’t spread, but because it was grade 3, the doctor recommended I have chemotherapy and radiation therapy.”
Julie
Taking care of yourself at home after a hysterectomy
Your recovery time will depend on the type of surgery you had, your age and general health. In most cases, you will feel better within 1–2 weeks and should be able to fully return to your usual activities after 4–8 weeks.
Rest up – When you get home from hospital, you will need to take things easy for the first week. Ask family or
friends to help you with chores so you can rest as much as you need to.
Nutrition – To help your body recover from surgery, eat a well-balanced diet that includes a variety of foods. Include proteins such as lean meat, fish, eggs, milk, yoghurt, nuts, and legumes/beans.
Work – You will probably need 4–6 weeks of leave from work, depending on the type of surgery and nature of your job. People who have had keyhole surgery and have office jobs that don’t require heavy lifting can often return to work after 2–4 weeks.
Driving – You will need to avoid driving after the surgery until you are able to move freely without pain. Discuss this issue with your doctor. Check with your car insurer for any exclusions regarding major surgery and driving.
If you don’t have support from family, friends or neighbours, ask your nurse or a social worker at the hospital whether it is possible to get help at home while you recover.
Lifting – You may be advised to avoid heavy lifting (more than 3–4 kg) for 4–6 weeks. This will depend on the way the surgery was done.
Bowel problems – It is important to avoid straining during bowel movements (pooing). Talk to your treatment team about the best way to manage constipation.
Bathing – Your doctor may advise taking showers instead of baths for 4–5 weeks after surgery.
Exercise – Your treatment team will probably encourage you to walk the day of the surgery. Exercise has been shown to help people manage some treatment side effects and speed up a return to usual activities. Speak to your doctor about suitable exercise. To avoid infection, it’s best to avoid swimming for 4–5 weeks after surgery.
Sex – Sexual intercourse should be avoided for about 6–12 weeks after surgery. Ask your doctor or nurse when you can have sex again, and explore other ways you and your partner can be intimate, such as massage.
Side effects after surgery
Menopause – If your ovaries are removed and you have not been through menopause, removal will cause immediate menopause. Menopause can cause significant emotional and physical changes.
Impact on sex and intimacy – The changes you experience after surgery may affect how you feel about sex. You may notice changes such as vaginal dryness and loss of libido. If you have concerns, you may find it helpful to talk to a psychologist or counsellor.
Lymphoedema – The removal of lymph nodes from the pelvis can stop lymph fluid draining normally, causing swelling in the legs or, sometimes, the vulva. This is known as lymphoedema. The risk of developing lymphoedema is low after most operations for cancer of the uterus, but the risk is higher if you have had a full lymphadenectomy followed by external beam radiation therapy. Symptoms may appear gradually, sometimes years after the treatment.
Vaginal vault prolapse – This is when the top of the vagina drops towards the vaginal opening because the structures that support it have weakened. Having a hysterectomy does not appear to increase the risk of vaginal vault prolapse in women without pelvic floor issues. Prolapse is more commonly caused by childbirth and weak pelvic floor muscles. Doing pelvic floor exercises several times a day can help to prevent prolapse. Talk to your treatment team about doing these exercises.
Find out more about the types of treatments:
Sources and references
This edition has been developed by Cancer Council NSW on behalf of all other state and territory Cancer Councils as part of a National Cancer Information Subcommittee initiative. All updated content has been clinically reviewed by Professor Alison Brand, Clinical Professor, The University of Sydney and Director, Department of Gynaecological Oncology, Westmead Hospital, NSW. This edition is based on the previous edition, which was reviewed by the following panel: A/Prof Orla McNally, Consultant Gynaecological Oncologist, Director Oncology/Dysplasia, Royal Women’s Hospital, Honorary Clinical Associate Professor, University of Melbourne, and Director of Gynaecology Tumour Stream, Victorian Comprehensive Cancer Centre, VIC; A/Prof Yoland Antill, Medical Oncologist, Peninsula Health, Parkville Familial Cancer Centre, Cabrini Health and Monash University, VIC; Grace Guerzoni, Consumer; Zeina Hayes, 13 11 20 Consultant, Cancer Council Victoria; Bronwyn Jennings, Gynaecology Oncology Clinical Nurse Consultant, Mater Hospital Brisbane, QLD; A/Prof Christopher Milross, Director of Mission and Radiation Oncologist, Chris O’Brien Lifehouse, NSW; Mariad O’Gorman, Clinical Psychologist, Liverpool Cancer Therapy Centre and Bankstown Cancer Centre, NSW. We would like to thank all the health professionals, consumers and editorial teams who have worked on current and previous editions of this title.
Cancer Council 13 11 20
Call us to talk to a specially trained health professional for free and confidential support and information.



