Last updated:
Sources and references What is testicular cancer?
Testicular cancer is not a common cancer but it is the second most common cancer in young men (aged 20 to 39) excluding non-melanoma skin cancer.
The most common testicular cancers are germ cell tumours. There are two main types, seminoma and non-seminoma. Seminoma usually occurs in men aged between 25 and 45 years and tends to develop more slowly than non-seminoma cancers. Non-seminomasare more common in younger men, usually in their late teens or early 20s.
It is estimated that 1,026 people were diagnosed with testicular cancer in 2024. The average age at diagnosis is 36 years old.
Testicular cancer signs and symptoms
Testicular cancer may cause no symptoms. The most common symptom is a painless swelling or a lump in a testicle or a change in size or shape.
- Less common symptoms include:
- feeling of heaviness in the scrotum
- feeling of unevenness
- pain or ache in the lower abdomen, the testicle or scrotum
- back pain
- enlargement or tenderness of the breast tissue (due to hormones created by cancer cells)
If found early, testicular cancer is one of the most curable cancers. This is why self-checking in so important.
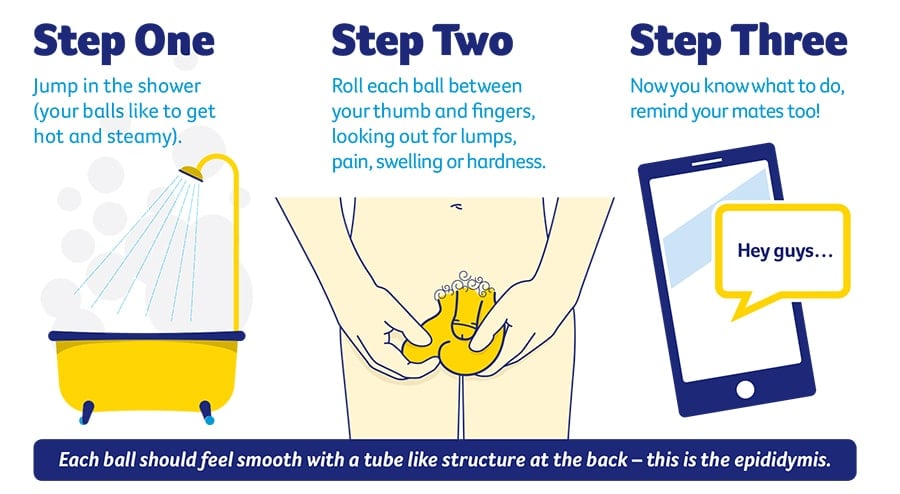
Image credit: Cancer Council Tasmania
Causes of testicular cancer
Some factors that may increase risk of testicular cancer include:
- undescended testicle (when an infant)
- family history (having a father or brother who has had testicular cancer)
- personal history – if you have had cancer in one testicle you are more likely to develop cancer in the other testicle
- infertility
- HIV and AIDS
- Physical features – people born with Hypospadias, which causes the urethra to open on the underside of the penis, are at an increased risk of testicular cancer
- Cannabis use – there is some evidence linking regular cannabis use to the development of testicular cancer
- Intersex variations - risk is higher in people with some intersex variations, such as partial androgen insensitivity syndrome
There is no known link between testicular cancer and injury to the testicles, sporting strains, hot baths or wearing tight clothes.
Diagnosis of testicular cancer
If you notice any changes, you should visit your GP who will examine your testicles for any lumps or swelling. Other tests used to diagnose testicular cancer include:
Ultrasound
To confirm the presence of a mass.
Blood tests
Blood tests for the tumour markers alpha-fetoprotein, beta human chorionic gonadotrophin and lactate dehydrogenase.
Surgery
The only way to definitely diagnose testicular cancer is by surgical removal of the affected testicle. While many other types of cancers are diagnosed by biopsy (removing a small piece of tissue from the tumour), cutting into a testicle could spread the cancer to other parts of the body. Hence the whole testicle needs to be removed if cancer is strongly suspected.
After a diagnosis of testicular cancer
After finding out you have testicular cancer, you may feel shocked, confused, anxious or upset. These are normal reactions and a diagnosis of testicular cancer affects everyone in different ways.
It can be difficult to decide what type of treatment to have. Understanding the disease, the treatments available and possible side effects can help you weigh up your options. You may also want to talk to your doctor about how treatment for testicular cancer may affect your fertility.
Treatment for testicular cancer
Staging
In addition to the results of the diagnostic tests above, a chest x-ray and CT scans of the chest, abdomen and pelvis are done to determine whether and how far the cancer has spread.
Stage 1 means the cancer is found only in the testicle, stage 2 means it has spread to the lymph nodes in the abdomen or pelvis, and stage 3 means the cancer has spread beyond the lymph nodes to other areas of the body such as the lungs and liver.
If the cancer is found only in the testicle (stage 1), removal of the testicle (orchidectomy) may be the only treatment needed. If the cancer has spread beyond the testicle, chemotherapy and/or radiation therapy may be used as well.
Palliative care
In some cases of testicular cancer, your medical team may talk to you about palliative care. Palliative care aims to improve your quality of life by alleviating symptoms of cancer.
As well as slowing the spread of testicular cancer, palliative treatment can relieve pain and help manage other symptoms. Treatment may include radiation therapy (radiotherapy), chemotherapy or other drug therapies.
Treatment Team
Depending on your treatment, your treatment team may consist of a number of different health professionals, such as:
GP (General Practitioner) - looks after your general health and works with your specialists to coordinate treatment.- Urologist - specialises in the treatment of diseases of the urinary system (male and female) and the male reproductive system
- Medical oncologist - prescribes and coordinates the course of chemotherapy.
- Radiation oncologist - prescribes and coordinates radiation therapy treatment.
- Cancer nurse - assists with treatment and provides information and support throughout your treatment.
- Other allied health professionals - such as social workers, pharmacists, and counsellors
Screening for testicular cancer
There is no routine screening test for testicular cancer. While it is important to get to know the regular look and feel of your testicles and let your doctor know if you notice anything unusual, there is little evidence to suggest that testicular self-examination detects cancer earlier or improves outcomes.
Preventing testicular cancer
There are no proven measures to prevent testicular cancer.
Prognosis for testicular cancer
Prognosis means the expected outcome of a disease. An individual's prognosis depends on the type and stage of cancer as well as their age and general health at the time of diagnosis. You may wish to discuss your prognosis and treatment options with your doctor, but it is not possible for any doctor to predict the exact course of your disease.
All testicular cancers can be treated and most testicular cancers are successfully treated.
Sources and references
- Understanding Testicular Cancer, Cancer Council Australia, © 2023. Last medical review of source booklet: August 2023. We thank the reviewers of this booklet: Dr Benjamin Thomas, Urological Surgeon, The Royal Melbourne Hospital and The University of Melbourne, VIC; A/Prof Ben Tran, Genitourinary Medical Oncologist, Peter MacCallum Cancer Centre, Walter and Eliza Hall Institute of Medical Research and The University of Melbourne, VIC; Dr Nari Ahmadi, Urologist and Urological Cancer Surgeon, Chris O’Brien Lifehouse, NSW; Helen Anderson, Genitourinary Cancer Nurse Navigator, Gold Coast University Hospital, QLD; Anita Cox, Youth Cancer – Cancer Nurse Coordinator, Gold Coast University Hospital, QLD; Dr Tom Ferguson, Medical Oncologist, Fiona Stanley Hospital, WA; Dr Leily Gholam Rezaei, Radiation Oncologist, Chris O’Brien Lifehouse and Royal Prince Alfred Hospital, NSW;Dheeraj Jain, Consumer; Amanda Maple, 13 11 20 Consultant, Cancer Council SA; Jessica Medd, Senior Clinical Psychologist, Department of Urology, Concord Repatriation General Hospital and Headway Health, NSW.
- Australian Institute of Health and Welfare. Cancer data in Australia [Internet]. Canberra: Australian Institute of Health and Welfare, 2024 Available from: https://www.aihw.gov.au/reports/cancer/cancer-data-in-australia
Cancer Council 13 11 20
Call us to talk to a specially trained health professional for free and confidential support and information.



