What is environmental tobacco smoke?
Burning tobacco products produces two types of smoke:
- side-stream smoke (smoke released from the tip of the cigarette)
- mainstream smoke (smoke exhaled by the smoker).
The combination of these two types of smoke is called environmental tobacco smoke and is also known as second-hand smoke. ‘Passive smoking’ is the inhalation of second-hand smoke.
Second-hand smoke is a carcinogen, meaning it is known to cause cancer as it contains around 7000 chemicals, 69 of which are known to cause cancer on their own.
There is no safe level of exposure to second-hand smoke. Second-hand smoke has been shown to be harmful even at low levels, including in outdoor areas.
Second-hand smoke and cancer
Second-hand smoke increases your risk of experiencing short-term health problems, including headaches and irritation of the eyes, nose and throat. The risk of serious long-term health issues are also increased; these include lung cancer, diseases of the heart and blood vessels and possibly stroke, nasal sinus cancer, breast cancer and chronic obstructive pulmonary disease (COPD).
Second-hand smoke has also been linked to the onset of adulthood asthma, poorer mental health and as a cause of early death.
In 2004-2005 it was estimated that 141 Australian deaths were due to inhaling second-hand smoke and in 1998 around 500 adults were admitted to hospital due to complications caused by second-hand smoke.
Your cancer risk from second-hand smoke varies depending upon:
- the length of exposure
- the concentration of toxins in the second-hand smoke
- how ‘old’ the second-hand smoke is
- the size of the space
- the ventilation rate
- the number of cigarettes being smoked at the same time by different people in the same area
- if you are a smoker or non-smoker, as non-smokers are more sensitive to damage (however, second-hand smoke is harmful to everyone)
Why second-hand smoke is harmful
Side-stream smoke is made at lower temperatures than mainstream smoke. As a result, it contains a higher amount of some toxins compared to the smoke being inhaled by the smoker. Some of these toxins in second-hand smoke are smaller than those being inhaled by the smoker. This means the smoke can go deeper into the lungs and is more toxic. Additionally, half of the chemicals in the smoke can still be in the air five to six hours after it was first created.
It has been estimated that aged side-stream smoke is approximately 12 times more toxic than mainstream smoke. Although non-smokers inhale much less smoke than smokers, by mass second-hand smoke is more toxic than inhaled mainstream smoke. Therefore, smoking should never occur in enclosed workspaces, even if no one else is around.
Non-smokers exposed to second-hand smoke in the home have a 25-30% greater chance of developing heart disease and a 20-30% increased risk of developing lung cancer compared with people who live in a smoke-free home. It is suggested those exposed in the workplace have a similar increased risk.
Additionally, non-smokers who inhale second-hand smoke are at risk of many of the same tobacco-related diseases and health problems as smokers. Therefore, it is essential that regulations are in place to protect workers from exposure to second-hand smoke.
Occupational Cancer Risk Series - Environmental Tobacco Smoke
Benefits of a smoke-free workplace
Besides following work health and safety obligations, a smoke-free workplace also results in large benefits to the employer.
A smoke-free work place can:
- improve employee health
- increase productivity of workers (fewer/no smoking breaks)
- reduce sick leave due to illnesses linked to smoking and passive smoking
- decrease the number of staff retiring earlier than expected
- reduce cleaning and maintenance costs
- reduce fire hazard risk
- create a healthy business image
- support current smokers to cut down and quit
- result in a decrease in uptake among younger workers
Effective controls
All Australian workplaces must follow work health and safety laws. These vary slightly between states and territories, but the duty of care for employers and responsibilities of workers across Australia is similar:
- Employers are required to ensure the health and safety of their workers at their workplace.
- Workers must take care of their own health and safety.
- Workers must not negatively affect the health and safety of other people.
- Workers must follow any reasonable instruction and workplace health and safety policies.
- There are also environments that must be smoke-free.
Western Australia’s Work Health and Safety (General) Regulations 2022 outline that employers, employees and the self-employed are not to smoke in indoor workplaces (this includes vehicles). If caught smoking in an enclosed workplace the person responsible and the person in control of the workplace can be fined or prosecuted.
Safe Work Australia and the Department of Health both outline how workers exposure to second-hand smoke in the workplace can be controlled. A summary of recommended controls is outlined in Table 1, but the full documents should be read for further detail. A combination of controls should be used.
If adequate control measures are not in place, anyone working around second-hand smoke is at increased risk of developing health problems, including cancer.
To follow work health and safety laws employers should eliminate or reduce exposure to identified hazards using the hierarchy of control (Figure 1) and implement a risk management process. Workers should always be involved in this process to correctly detect hazards and put in place control measures that suit the workplace. Training workers on the hazards present in the workplace and the procedures used to manage them is also a work health and safety requirement.
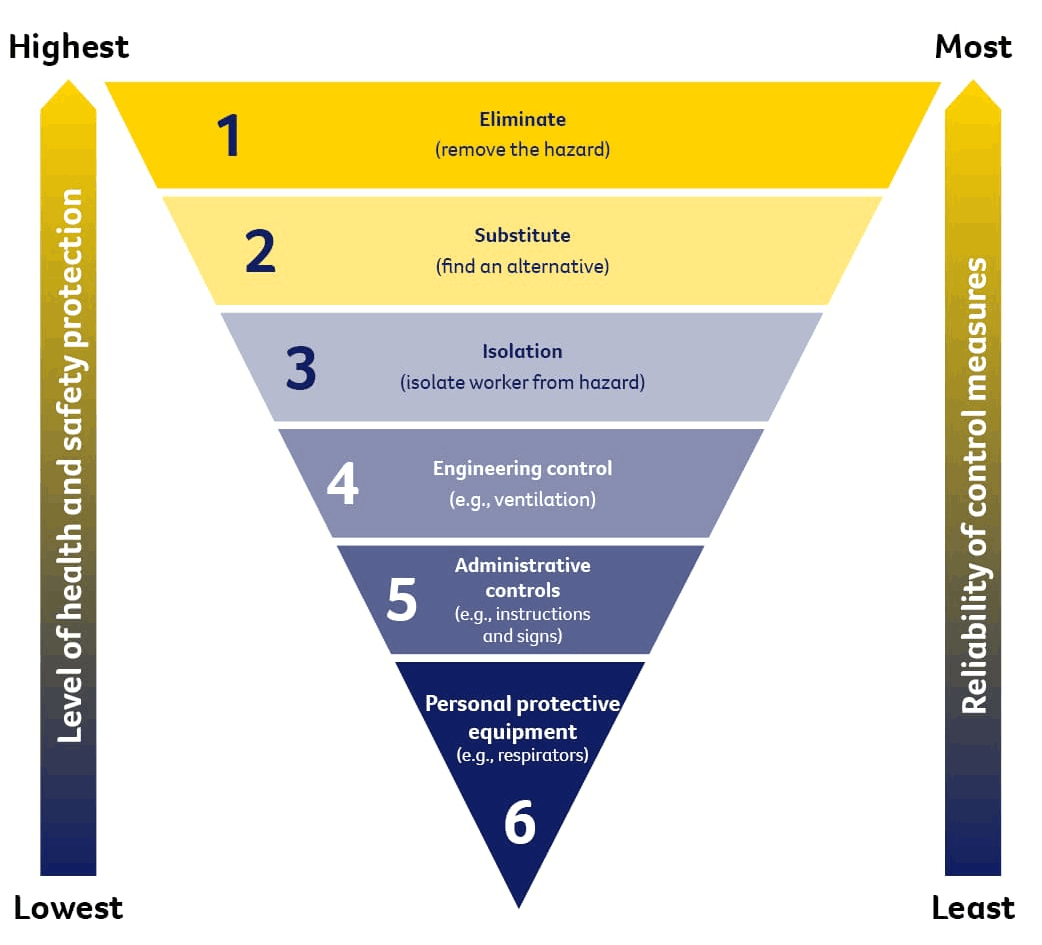
Figure 1. The hierarchy of risk control
Table 1. Summary of second-hand smoke exposure control measures
| ACTIVITY CONTROL | CONTROL |
| Banning smoking in the workplace | This should include indoor areas, in vehicles, enclosed and partially enclosed areas and outdoor areas where smoke can drift into the workplace. |
| Having in place a written no-smoking/second-hand smoke policy | A second-hand smoke policy should be developed that includes education on tobacco control methods and safe work practices. This will explain how and why second-hand smoke needs to be managed. It is also an effective tool in reducing smoking among employees and is an important step to becoming a smoke-free workplace. A sample second-hand smoke policy is available at Department of Health WA's Supporting a smoke-free workplace - a policy implementation guide (page 21). |
| Provide cessation (quit) support and programs | To encourage employees to quit, a supportive environment is required, including a positive attitude from management and coworkers. Employers can provide information resources, self-help materials, encourage employees to use the Quitline (13 78 48), the QuitCoach or My QuitBuddy. Additionally, workplace quit programs can be offered to employees. For more information about workplace programs (or cessation information), please contact your state or territory Cancer Council office. |
| Designated smoking areas | Designated smoking areas must be outdoors well away from doorways, windows and ventilation ducts, e.g. at least 5 metres from doorways and windows and 10 metres from ventilation ducts. This is so drift to other areas of the workplace cannot occur. Outdoor levels of second-hand smoke can be similar to those of indoor concentrations, under certain conditions, when people are smoking. Designated smoking areas in indoor areas of the workplace is prohibited by law even if ventilated. The use of the designated smoking area can be restricted to certain times, e.g. award meal breaks. It is recommended smoking be prohibited in all work areas. |
| Signage | Using signs with standard symbols indicate to the staff and visiting people that workplace areas are non-smoking. You can order this signage from your state government's tobacco compliance department. |
For any concerns related to smoking at your workplace, contact:
- your workplace supervisor or management (if you are an employee)
- your workplace health and safety representative or union representative
- state and territory work health and safety regulators
- Safe Work Australia
How do I detect cancer early and reduce my cancer risk?
If you think you may have been exposed to a cancer-causing agent, it is important to speak with a GP or health professional.
To find out what you can do to create a workplace that supports healthy choices to help reduce cancer risk, contact Cancer Council 13 11 20.
Sources
- National Occupational Health & Safety Commission. Guidance note on the elimination environmental tobacco smoke in the workplace 2003. National Occupational Health & Safety Commission Canberra, ACT.
- International Agency for Research on Cancer. IARC Monographs on the Evaluation of Carcinogenic Risks to Humans: Tobacco Smoke and Involuntary Smoking 2004. International Agency for Research on Cancer Lyon, France
- U.S. Department of Health and Human Services. How Tobacco Smoke Causes Disease: The Biology and Behavioral Basis for Smoking-Attributable Disease: A Report of the Surgeon General. 2010, U.S. Department of Health and Human Services.
- United States Department of Health and Human Services. The Health Consequences of Involuntary Exposure to Tobacco Smoke: A Report of the Surgeon General. 2006.
- WHO Regional Office for Europe. Air quality guidelines for Europe 2000. WHO Regional Publications Copenhagen.
- United States Environmental Protection Agency. Respiratory Health Effects of Passive Smoking: Lung Cancer and Other Disorders. 1992, United States Environmental Protection Agency: Washington DC. p. 63.
- California Environmental Protection Agency. Health Effects of Exposure to Environmental Tobacco Smoke. Tobacco Control, 1997. 6(4): p. 346-353.
- Council, N.H.a.M.R. The Health Effects of Passive Smoking: A Scientific Information Paper. 1997, Commonwealth of Australia: Canberra, ACT.
- Cao, S., et al. The Health Effects of Passive Smoking: An Overview of Systematic Reviews Based on Observational Epidemiological Evidence. PLoS ONE, 2015. 10(10): p. e0139907.
- U.S. Department of Health and Human Services. The Health Consequences of Involuntary Smoking. U.S. Department of Health and Human Services, et al., Editors. 1986, US Government Printing Office: Washington DC.
- Partnership, N.P.H., National response to passive smoking in enclosed public places and workplaces A Background Paper. 2000, Commonwealth of Australia: Canberra, ACT.
- Fischer, F. and Kraemer, A. Meta-analysis of the association between second-hand smoke exposure and ischaemic heart diseases, COPD and stroke. BMC Public Health, 2015. 15: p. 1202.
- Malek, A.M., et al. Secondhand Smoke Exposure and Stroke: The Reasons for Geographic and Racial Differences in Stroke (REGARDS) Study. American Journal of Preventive Medicine, 2015. 49(6): p. e89-e97.
- Ye, X., et al. Dose-response relations between second-hand smoke exposure and depressive symptoms among middle-aged women. Psychiatry Research, 2015. 229(1-2): p. 533-538.
- Yang, T., et al. Second hand smoke exposure in public venues and mental disorder: a representative nationwide study of China. Tobacco Induced Diseases, 2015. 13(1): p. 1-8.
- Zeng, Y.N. and Li, Y.M. Secondhand smoke exposure and mental health in adults: a meta-analysis of cross-sectional studies. Social Psychiatry and Psychiatric Epidemiology, 2015: p. 1-10.
- Lv, X., et al. Risk of all-cause mortality and cardiovascular disease associated with secondhand smoke exposure: A systematic review and meta-analysis. International Journal of Cardiology. 199: p. 106-115.
- Collins, D. and H. Lapsley, The costs of tobacco, alcohol and illicit drug abuse to Australian society in 2004-05, C.D.o.H.a. Ageing, Editor. 2008, Department of Health and Ageing: Canberra, ACT.
- Ridolfo, B. and Stevenson, C. Quantification of drug-caused mortality and morbidity in Australia, 1998-2001. Australian Institute of Health and Welfare Canberra.
- Davis, R. Exposure to Environmental Tobacco Smoke: Identifying and Protecting Those At Risk. The Journal of the American Medical Association, 1998. 280(22): p. 1947-1949.
- Schick, S. and Glantz, S.A. Sidestream cigarette smoke toxicity increases with aging and exposure duration. Tobacco Control, 2006. 15(6): p. 424-429.
- Valavanidis, A., Fiotakis K. and Vlachogianni, T. Airborne particulate matter and human health: toxicological assessment and importance of size and composition of particles for oxidative damage and carcinogenic mechanisms. J Environ Sci Health C Environ Carcinog Ecotoxicol Rev, 2008. 26(4): p. 339-62.
- Halpern, M.T., et al. Impact of smoking status on workplace absenteeism and productivity. Tobacco Control, 2001. 10(3): p. 233-238.
- Collins, D., Lapsley, HM. Economic costs of Alcohol and other Drugs in the Workplace. 1st ed. 2001, Adelaide National Centre for Education and Training on Addiction.
- Cheng, K.W., et al. The Effects of Workplace Clean Indoor Air Law Coverage on Workers' Smoking-Related Outcomes. Health Economics, 2015: p. n/a-n/a.
- Jones, M.R., et al. Cardiovascular Events Following Smoke-Free Legislations: An Updated Systematic Review and Meta-Analysis. Current environmental health reports, 2014. 1(3): p. 239-249.
- Scollo, M. and Winstanley, M. Tobacco in Australia: Facts and issues. 2015. Cancer Council Victoria: Melbourne, Victoria.
- Zablocki, R.W., et al. Smoking ban policies and their influence on smoking behaviors among current California. 2013. Elsevier.

